The Return of Measles: Causes Behind the Global Surge in Cases
Measles cases are rising globally due to declining vaccination rates, pandemic-related disruptions, and increased international travel.
Mar 17, 2026
Once considered nearly eliminated in many parts of the world, Measles is re-emerging as a significant public health issue. Recent data from international health organizations, including the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC), indicate a steady rise in measles cases across multiple regions. This resurgence highlights gaps in immunization coverage and the consequences of disrupted healthcare systems.
Measles is a highly contagious viral disease caused by the measles virus, which spreads through respiratory droplets when an infected person coughs or sneezes. The virus can remain active in the air or on surfaces for up to two hours. Due to its high transmissibility, measles has a basic reproduction number (R₀) estimated between 12 and 18, meaning one infected individual can spread the virus to many others in a susceptible population.
Rising Global Cases
After a decline in measles cases during the early 2000s due to widespread vaccination campaigns, global numbers have begun to rise again. According to WHO estimates, there were approximately 9 million measles cases worldwide in 2021, resulting in around 128,000 deaths, primarily among children under five. More recent estimates suggest that infections increased further, reaching approximately 11 million cases globally in 2024.
The Americas, which had previously achieved measles elimination status in 2016, have reported a sharp increase in cases in recent years. Data from the Pan American Health Organization (PAHO) shows that measles cases in the region rose significantly between 2024 and 2025, with some countries reporting outbreaks linked to declining vaccination coverage. Similarly, outbreaks have been reported across Europe, Asia, and parts of Africa, indicating that the resurgence is not confined to a single geographic area.
Decline in Vaccination Coverage
A key factor contributing to the return of measles is the decline in routine immunization rates. The measles-containing vaccine, commonly administered as part of the MMR (measles, mumps, and rubella) vaccine, is highly effective. Two doses provide approximately 97% protection against the disease.
To prevent outbreaks, at least 95% of the population must be vaccinated to achieve herd immunity. However, global vaccination coverage has fallen below this threshold in many countries. WHO and UNICEF reported that in 2022, approximately 25 million children missed at least one routine vaccine dose, the highest number in over a decade. This created a large pool of susceptible individuals, increasing the risk of outbreaks.
Impact of the COVID-19 Pandemic
The COVID-19 pandemic played a major role in disrupting routine immunization services worldwide. Lockdowns, healthcare system strain, and reduced access to medical facilities led to missed vaccination appointments for millions of children. According to global health agencies, over 60 million routine vaccine doses were delayed or missed between 2020 and 2022. These disruptions created immunity gaps in many populations. As countries resumed normal activities and international travel increased, the measles virus was able to spread more easily among unvaccinated groups.
Role of International Travel
Global travel has also contributed to the spread of measles. The virus is frequently imported into countries through travelers who contract the disease in regions where measles remains endemic. Even countries with high vaccination coverage can experience outbreaks if pockets of unvaccinated individuals exist.
Health authorities often trace outbreaks back to imported cases, followed by local transmission within communities with low immunization rates. This pattern has been observed in multiple recent outbreaks across North America, Europe, and Asia.
Clinical Features and Complications
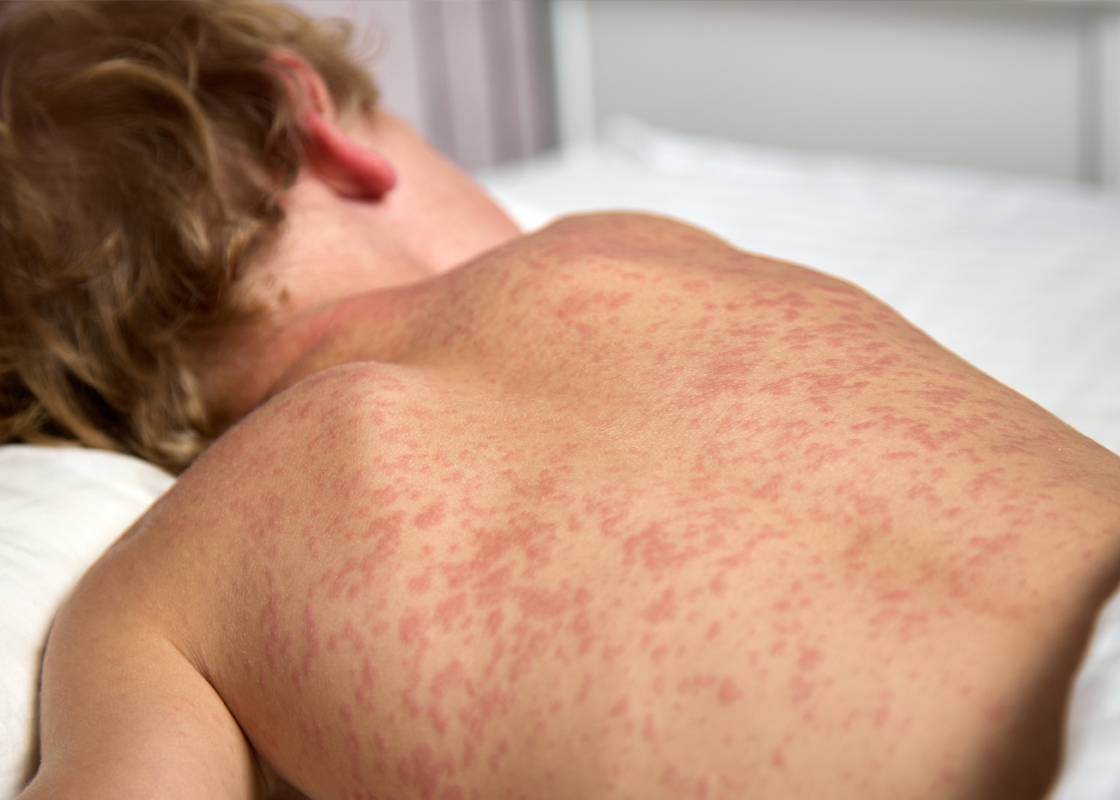
Measles typically begins with symptoms such as high fever, cough, runny nose, and conjunctivitis (red, watery eyes). A characteristic red rash appears several days later, usually starting on the face and spreading to the rest of the body.
While many cases resolve without complications, measles can lead to serious health issues. Common complications include ear infections and diarrhea. More severe outcomes include pneumonia, which is the leading cause of measles-related deaths, and encephalitis, a form of brain inflammation that can result in permanent neurological damage. According to WHO data, approximately 1 in 5 unvaccinated individuals in high-income countries who contract measles require hospitalization.
Prevention and Control Measures
Vaccination remains the most effective method of preventing measles. The MMR vaccine has been widely used for decades and has a strong safety and efficacy profile. Public health strategies to control measles include routine immunization programs, supplementary vaccination campaigns, and rapid response to outbreaks.
Surveillance systems are also critical for detecting and responding to measles cases. Many countries maintain laboratory-confirmed reporting systems to track outbreaks and implement containment measures such as isolation and contact tracing.
The resurgence of measles is closely linked to declining vaccination coverage, disruptions caused by the COVID-19 pandemic, and increased global mobility. Despite being preventable through vaccination, measles continues to pose a significant threat to public health worldwide. The recent rise in cases underscores the importance of maintaining high immunization rates and strengthening healthcare systems to prevent further outbreaks.




